Degenerative Disc Disease Treatment in Arizona – Gilbert, Chandler, Mesa, Queen Creek
Degenerative disc disease (DDD) is a condition caused by wear and tear of the spinal discs, which usually is the result of aging. The discs between the vertebrae (spinal bones) are what allows us to bend, flex, and even twist and turn without pain or harm to our body. The intervertebral (between 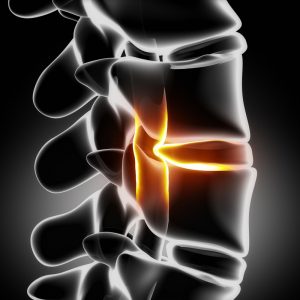 vertebra) discs are like shock absorbers between the bones of the spine, and they are designed to help our back to handle forces and stay flexible.
vertebra) discs are like shock absorbers between the bones of the spine, and they are designed to help our back to handle forces and stay flexible.
MRI studies show that most everyone older than 60 years has some degree of degenerative disc disease. Many people have back pain with this condition, but some do not. When the discs rub against each other, it can cause the pain and stiffness which we call osteoarthritis, as well as spinal nerve compression that causes shooting and stabbing pain.
Incidence
The lifetime incidence of low back pain is around 75%, and the annual occurrence rate is 5%. Every year, 14% of new patients visit a doctor for low back pain, and many of these people have degenerative disc disease. In one study, 33% of patients with low back pain suffered discomfort for less than one month, but 33% also had it for longer than six months.
Causes
Degenerative disc disease isn’t actually considered a disease at all. It’s a condition in which pain is caused from a disc that loses its ability to function properly. Here are reasons why discs may degenerate:
- Age
- Disc drying out due to aging
- Sports/daily activities which can cause tears on outer core of disk
- Injuries from any source
Symptoms
Symptoms of degenerative disc disease usually involve pain in the neck or lower back. Here are some common symptoms associated with DDD: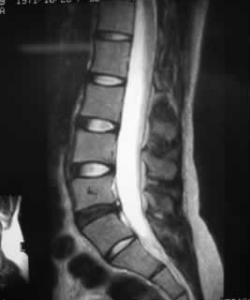
- Neck pain which usually radiates to the arms and hands.
- Lower back pain which affects the buttocks and thighs.
- Pain while sitting.
- Pain that irritates when twisting, bending or lifting.
- Pain that comes and goes, mostly severe, and lasting from days to months.
- Tingling or numbness in hands and feet.
- Pain that goes away when moving around, walking, laying, and moving positions.
- Weakness in leg muscles due to damage to nerve root, also losing foot control.
Diagnosis
When having degenerative disc disease diagnosed, it will require a physical examination. You will also be questioned about your medical history, which will include a description of your symptoms, when they began, and where the pain started. There are tests, such as an MRI or x-rays, which will show damage to discs but won’t confirm the condition.
Treatment
Exercise helps increase the flexibility and the strength of the muscles that surround and support the spine and is required by most doctors in order to get back, neck and surrounding pain under control. By exercising, we increase the blood flow to the back and other areas, and by 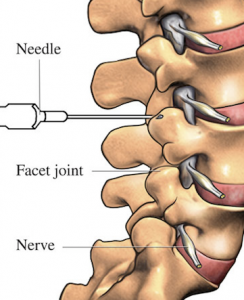 doing this, it helps nourish muscles and joints with nutrients and oxygen while helping to clear away inflammatory waste products. Here are some treatment ideas or options to help out with physical activity/exercises to increase back strength:
doing this, it helps nourish muscles and joints with nutrients and oxygen while helping to clear away inflammatory waste products. Here are some treatment ideas or options to help out with physical activity/exercises to increase back strength:
- Heat and cold therapy
- Physical therapy
- Pain relievers such as Tylenol (acetaminophen) and nonsteroidal anti-inflammatory drugs (naproxen sodium, ibuprofen) and others.
- Spinal mobilization
- Facet Blocks, Medial Branch Blocks
- Intradiscal Injections
- Radiofrequency Ablation
- Regenerative Medicine Injections – PRP and/or Stem Cell Therapy
- Surgery, which consist of spinal fusion and/or artificial disc replacement.
Dr. Ajay Yeddu offers comprehensive, exceptional treatment options for degenerative disc disease causing considerable back pain. This may include medication management and/or interventional procedures for patients in Gilbert, Chandler, Mesa, Queen Creek and Maricopa AZ. Most insurance is accepted, call us today!
Resources
Frymoyer JW. Epidemiology: the magnitude of the problem. In: Wiesel SW, Weinstein JN, Herkowitz HH, Dvorak J, eds. The Lumbar Spine. 2nd ed. Philadelphia, PA: WB Saunders Co. 1996.
Luo X, Pietrobon R, Sun SX. Estimates and patterns of direct health care expenditures among individuals with back pain in the United States. Spine. 2004 Jan 1. 29(1):79-86.